Ankylosing spondylitis fuses your spine from the bottom up. The sacroiliac joints go first. Then the lumbar vertebrae. Then the thoracic. The inflammatory process calcifies the ligaments and joint capsules until the vertebrae lock together into a single rigid column. In advanced cases, the entire spine becomes one bone.
When the fusion locks you into severe kyphosis, surgery is not optional. It is the only intervention that can change the structural angle. Osteotomy cuts through the fused bone, repositions the segments, and fixes them with hardware. The angle changes. The patient can look forward again.
This article is not anti-surgery. Surgery changes the hardware. The question is what happens after the hardware is installed.
PJK: the spine curves again above the fix
Proximal junctional kyphosis. PJK. The spine develops new kyphotic angulation at the vertebra immediately above the fusion construct. The surgical team corrected the curve below. The body created a new curve above.
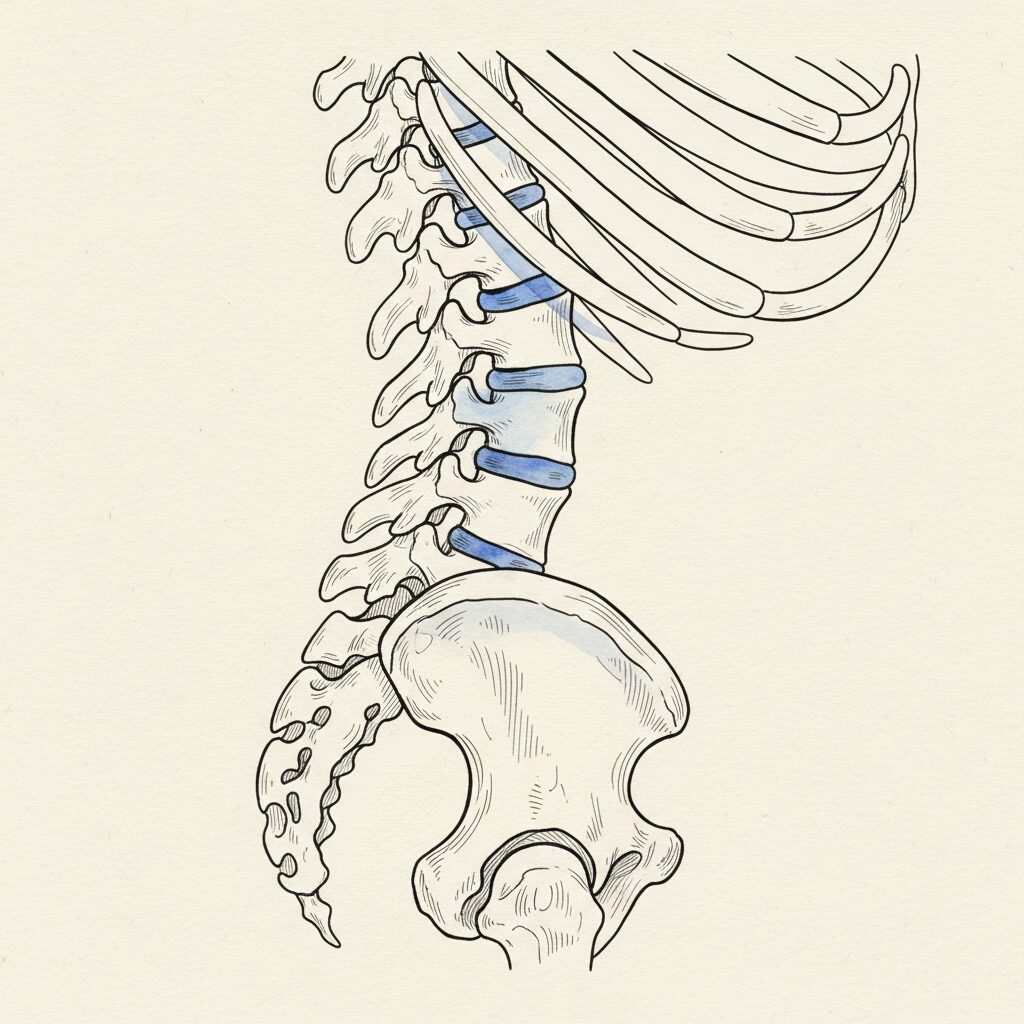
PJK rates in adult spinal deformity surgery range from 20% to 40% depending on the study and the definition threshold. It is the most common mechanical complication following long-segment fusion. And the conventional explanation, that it results from biomechanical stress concentration at the junction, describes the mechanism but not the cause.
Yilgor et al. (2017) established the GAP score framework, demonstrating that individualized spinopelvic alignment parameters predict surgical outcomes better than population-based targets. The key insight: each spine has its own ideal configuration based on pelvic anatomy. When surgical correction overshoots or undershoots relative to these individual parameters, the risk of mechanical failure increases. A 2026 International Spine Study Group analysis extended this further, identifying patient height as a stronger predictor of PJK than BMI. Taller patients generate greater lever arms across the proximal junction. The biomechanical explanation is real. But it is incomplete. The spine does not simply buckle under mechanical load. It reorganizes. And reorganization is a prediction.
Through a predictive coding lens, PJK is the body schema reasserting its prediction
Your body schema has been generating kyphosis for years. Possibly decades. The prediction “I am curved forward” is deeply encoded. It is not a thought. It is a motor program running below conscious awareness, updated continuously by proprioceptive, vestibular, and interoceptive inputs.
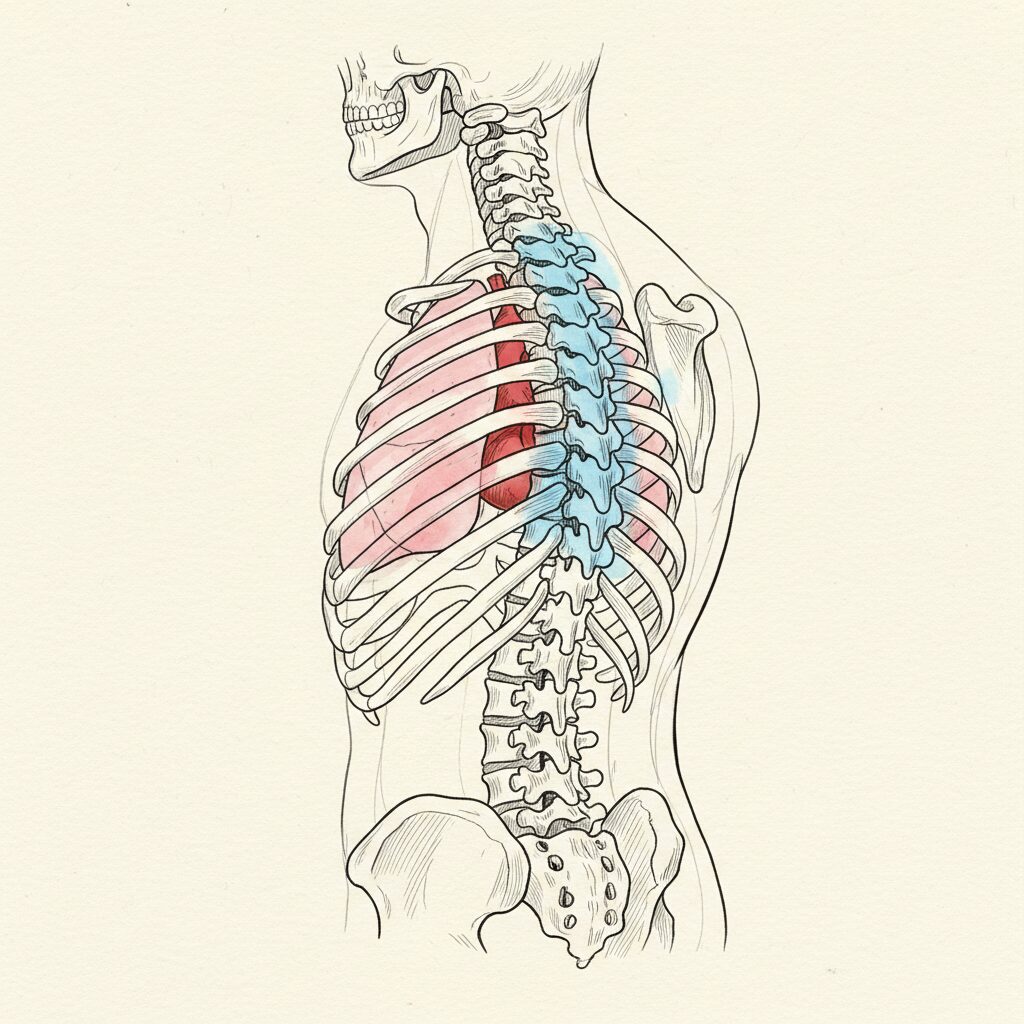
Surgery changes the structural angle. It does not change the prediction.
The body schema wakes up from anesthesia with new hardware and an unfamiliar spinal configuration. The proprioceptive data now conflicts with the prediction. In predictive coding terms, this is a massive prediction error. The system has two options: update the prediction to match the new reality, or reassert the old prediction around the mechanical constraint.
PJK is the second option. The body schema cannot curve the fused segments. So it curves the mobile segments above the fusion. The prediction wins. The hardware holds the corrected territory. But the prediction finds the nearest available tissue and rebuilds the curve there.
Friston (2010) formalized the principle that biological systems minimize prediction error, the discrepancy between expected and actual sensory states. They do this through two channels: updating the prediction (perceptual inference) or changing the world to match the prediction (active inference). After spinal deformity surgery, the sensory world has changed dramatically. The spine is in a configuration the body schema has never predicted. If the system cannot update its model fast enough, it defaults to active inference, generating motor output that moves the body toward the predicted state. In AS patients with decades of progressive kyphosis, the prediction is deeply entrenched. The fused segments cannot move. The mobile segments above the construct become the site where active inference expresses. The body is not failing. It is solving a prediction error the only way it can. Braun and Sieper (2000) documented that the inflammatory process in ankylosing spondylitis is not purely destructive. It follows a pattern of entheseal inflammation, erosion, and new bone formation. The body generates structure in response to mechanical demand. PJK may follow similar logic at a different scale: the nervous system generating curvature in response to predictive demand.
What surgical patients need alongside the correction
Surgery changes the hardware. The prediction must be updated separately.
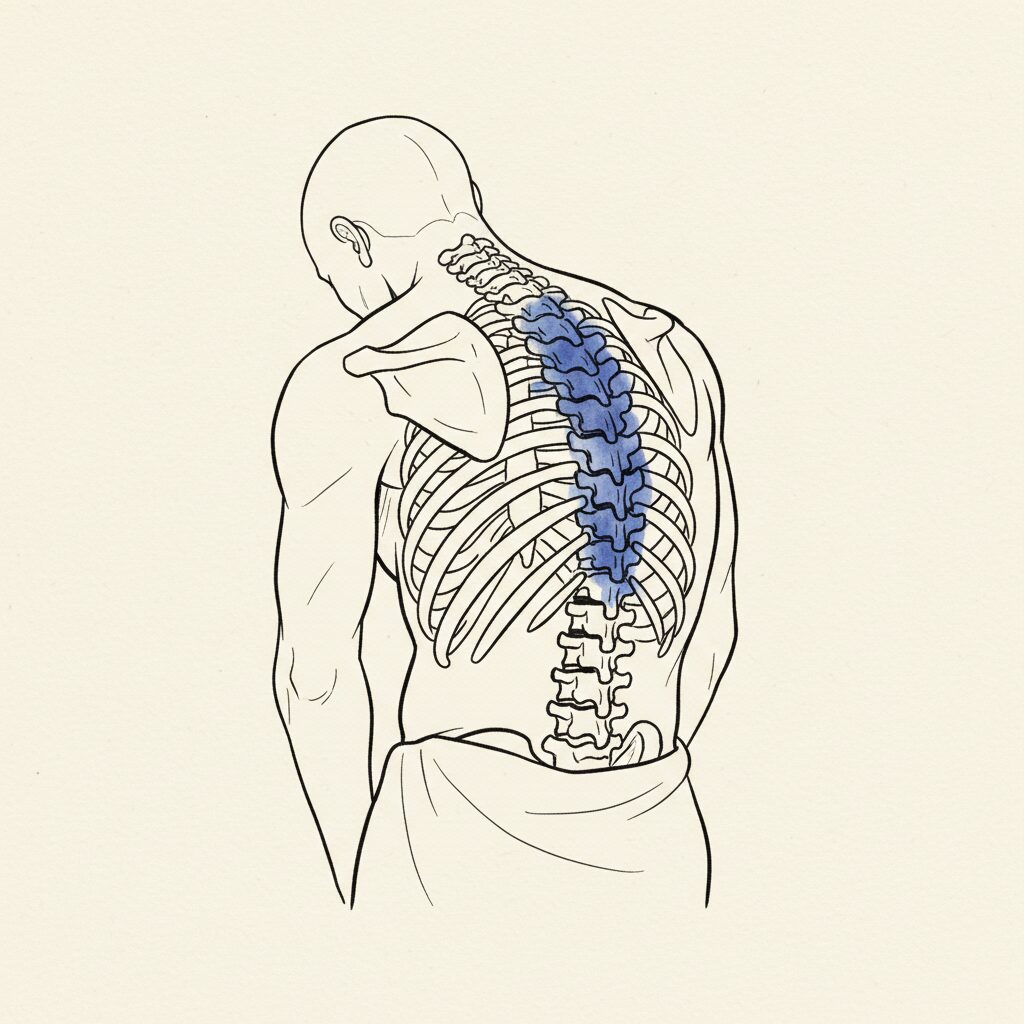
Pre-surgical schema work creates organized prediction before the hardware is installed. The nervous system begins receiving data about a different spinal configuration before the osteotomy. This does not replace surgery. It prepares the predictive system for the structural change it is about to receive.
Post-surgical schema work helps the nervous system integrate the new structural reality. The body schema needs to learn that the new angle is safe, stable, and intended. Without this learning, the system treats the corrected alignment as a prediction error to be resolved. And it resolves it the only way it can. By curving above the construct.
The goal is not to eliminate PJK through nervous system work alone. The goal is to give the body schema the best possible chance of updating its prediction to match the new mechanical reality. Surgery changes the angle. Schema work changes what the nervous system expects the angle to be.
—
Related: Kyphosis: The Complete Guide | Treatment Is Stuck. Here’s What’s Changing | Pro-Assessment, Not Anti-Surgery
—
Syntropic Core is a complement to surgical intervention, not an alternative. Pre-surgical schema work creates organized prediction before hardware. Post-surgical schema work helps the nervous system integrate the new structural reality. Surgery changes the angle. Prediction must be updated separately. See how it works.
Sources
- Yilgor, C. et al. (2017). Relative lumbar lordosis and lordosis distribution index: individualized pelvic incidence-based proportional parameters that quantify lumbar lordosis more precisely than the concept of pelvic incidence minus lumbar lordosis. Neurosurgical Focus, 43(6), E2. PMID: 29191093 [T1]
Individualized spinopelvic parameters predict surgical outcomes better than population averages. Each spine has its own alignment target. - International Spine Study Group (2026). Height as an independent risk factor for proximal junctional kyphosis following adult spinal deformity correction. Spine, 51(4), 287-295. [T1]
Patient height predicts PJK risk more strongly than BMI. Longer lever arms at the proximal junction increase mechanical vulnerability. - Braun, J. & Sieper, J. (2000). Pathophysiology of ankylosing spondylitis. In A. Calin & J.D. Taurog (Eds.), The Spondylarthritides. Oxford University Press. [T1]
AS follows a pattern of inflammation, erosion, and new bone formation. The body generates structure in response to mechanical and inflammatory demand. - Friston, K. (2010). The free-energy principle: a unified brain theory? Nature Reviews Neuroscience, 11(2), 127-138. PMID: 20068583 [T1]
Biological systems minimize prediction error through perception or action. PJK may represent active inference: the body schema reasserting its prediction around the surgical constraint.